In the previous issue of The Beat, senior management responsible for clinical care at the University of Ottawa Heart Institute offered a wide-ranging discussion of the state of cardiovascular medicine in “The Changing Cardiovascular Landscape.” Many of the themes and trends raised there are directly related to ongoing changes in the patient population. In this and the next issue, we take a closer look at aspects of “The Changing Cardiovascular Patient.”

Canada is in the midst of fundamental demographic shifts that are not only changing the face of the country but greatly impacting the nature of the cardiovascular patient population. Life expectancy has increased dramatically over the past century for both men and women, rising from about 60 years of age in the 1920s to more than 80 today. Consequently, adults older than 65 make up an increasing proportion of the Canadian population, from less than 5 per cent in the 1920s to almost 15 per cent today, and are expected to rise to more than 20 per cent by 2040.
An aging population alone would have major implications for the prevalence and treatment of heart disease. That shift, though, is accompanied by health trends that are directly associated with many cardiovascular risk factors. The news is more bad than good.
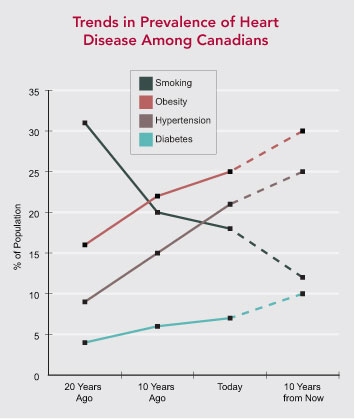
Between 1994 and 2005, the incidence of hypertension has jumped 8 per cent in the number of Canadians older than age 20 reporting high blood pressure. More and more Canadians are obese, with the Heart and Stroke Foundation recently predicting that by 2015, 20 to 30 per cent of men and 15 to 18 per cent of women will be obese.
According to the Canadian Diabetes Association, the number of Canadians with diabetes will rise from slightly more than 3 million today to more than 3.7 million by 2020. “We have definitely seen an increase in the prevalence of diabetes within our population,” confirmed Bonnie Quinlan, University of Ottawa Heart Institute advanced practice nurse for cardiology. “Diabetes is so common in patients with heart disease now that we test every patient upon admission to the Heart Institute. Approximately 50 per cent of our patients are diabetic, and we pick up about 10 to 15 per cent of patients on admission who do not even know they’re diabetic.”
“Most of these patients I see aren't just coming in with heart failure. They’re also coming in with high blood pressure, high cholesterol and diabetes.” – Dr. Haissam Haddad, Director, Heart Failure Program, UOHI

The one piece of solidly good news comes from the realm of smoking cessation. Due to aggressive nationwide anti-tobacco policies and cessation efforts, the number of smokers in all age groups continues to decline in Canada. In 1999, 21 per cent of the population smoked. By 2007, this had dropped to 15 per cent, and the trend is predicted to continue.
Hospitalization rates for cardiovascular disease of any type have been steadily declining since the 1980s, resulting in heart disease falling below cancer as the leading cause of death in Canada. Unfortunately, that positive trend is not expected to continue. Given the changing patient landscape, the Heart and Stroke Foundation projects that the total number of hospitalizations in Canada from ischemic heart disease, acute heart attack and stroke will rise significantly by 2025.
The Public Health Agency of Canada reports that the number of coronary artery bypass grafts, coronary angioplasties, valve surgeries and pacemaker implantations have risen substantially since 1995. The increase in valve and pacemaker procedures is to be expected with an aging population. The increase in bypasses and angioplasties is greatly responsible for the substantial drop in deaths from acute heart attacks in recent decades.
“We saw a revolution in managing heart attack beginning in the 1980s,” said Dr. Haissam Haddad, Director of the Heart Institute’s Heart Failure program and Medical Director of the Heart Transplantation program. “The main reason we now see more heart failure and patients with more complex heart disease is really life expectancy; the population is simply getting older.”
“Most of these patients I see aren’t just coming in with heart failure. They’re also coming in with high blood pressure, high cholesterol, and diabetes. This is the trend we’ve been seeing in the clinic for the past 10 years,” he continued.
Comprehensive Care
“Many of our patients today are older, sicker and have multiple co-morbidities, which obviously present increased challenges to the health care system and to their communities as well,” agreed Quinlan.
In response, “many of our approaches have become multidisciplinary in nature. Now, when patients are admitted, not only do they see their attending physician and nurse, but we have an entire team that’s able to meet their care needs,” she explained. “For example, for patients with congestive heart failure—a huge portion of the inpatients at the Heart Institute—it’s a chronic, lifelong condition requiring very precise medical and lifestyle management in order to control the effects of the disease.”
“These patients are all seen not just by their advanced practice nurse and their attending cardiologist but by specialists from other disciplines. This ensures that they have an understanding of how to manage food and fluid intake to prevent readmission to hospital. They’re seen by a physiotherapist on a daily basis to ensure that their general level of fitness doesn’t deteriorate.”
Such chronic conditions require a multi-disciplinary approach with systems and processes in place so that patients are managed in a standardized fashion. At the Heart Institute, patient education and telemonitoring are important tools for keeping heart failure patients out of the hospital. “We teach them to look for signs and symptoms that would require a change in their medication,” said Quinlan. “And we work closely with the telehealth home monitoring program, so when patients do go home, we’re able to continue to monitor them and provide corrective feedback to reduce the likelihood of readmission to hospital.”
According to Dr. Haddad, care for the older cardiovascular patient has improved in recent years thanks to advances in technology and surgical technique. “For example, instead of heart-valve replacement, in the past 15 or so years, we’ve started doing repair. We can do this on a lot of lower-functioning patients who before would not have been candidates for surgery.”
Another highly beneficial procedure for sicker patients, explained Dr. Haddad, is the implantable cardioverter defibrillator (ICD), which can monitor for abnormal heart rhythms and provide a shock to re-establish a normal rhythm. Use of this cardiac resynchronization therapy in specific patients improves survival rates and quality of life.
“With everything mentioned above, there is no age limit for such procedures; we base those decisions on co-morbidities, not age. Even for heart transplant our decision is based on symptoms, co-morbidities and the potential for a positive outcome. Will this patient benefit from the intervention? Does the data support it? If yes, then we’ll do it,” he explained.
Toward Holistic Care
The improvements in technology are unfortunately being counterbalanced by the increased prevalence in risk factors for heart disease. That overall increase in risk factors in the population has heightened the need for education, both for patients and their families, explained Quinlan. “Hospitalization is an ideal moment for teaching, not just patients but their families as well,” she said.
“In the classes I teach here every day, focusing on the prevention of coronary artery disease, I always encourage family members to attend. That way, we’re doing primary prevention as well as secondary prevention, hopefully keeping the next generation or two from entering our system earlier. I think that’s where we maybe need to put more of our efforts, capitalizing on the patient’s presence to reach others around them,” she continued.
Education in this context invariably involves more than a review of lifestyle factors. “People often ask about their genetic risk,” said Quinlan. “All of us have a genetic, family history of something. For many people, it is heart disease. The way we look at it in clinical practice is to tell them ‘Yes, you have a predisposition for developing, say, CAD [coronary artery disease], but there still is a lot within your control to change the course of the future by controlling these other risk factors.’ Research has shown that in all patient populations, significant risk reductions can be achieved by tightly controlling the modifiable risk factors. That’s an important message for patients.”
Once older patients leave the Heart Institute, they often face another challenge not often encountered by younger patients—isolation. “Our medical management is much better than 10 years ago, but our patients’ needs are not just medical,” said Dr. Haddad. “If you have an 85-year-old patient who has heart failure, from the medical point of view, we can stabilize them the same way as a 50-year-old patient. But these people mostly live alone; they don’t have the support that younger people may have.”
“It’s not enough just to see patients every three or six months and give them some instructions. People who have caregivers who can help look after their diets and medications do much better than people who live alone, who aren’t sure what they should be eating or if they should be exercising,” he continued.
“We need to work on infrastructure to provide the right support for the elderly population with chronic diseases. I think that’s more important right now than spending more money in the acute setting,” he speculated. “We have to have chronic disease management team support in the home environment, whether that’s a patient’s home, a family member’s home, or a nursing home. With better support, I think the outcomes would be much better in this population.”
A comprehensive, holistic approach to the care of cardiovascular patients will be increasingly important as heart disease continues its evolution from an acute, often fatal condition to a chronic disease to be managed over the rest of a patient’s lifetime—a chronic disease with a growing prevalence in the Canadian population.
In addition to more education and greater integrated support beyond the hospital environment, a comprehensive approach may also include expanded use of palliative care in the discipline and more recruitment of specialists into chronic disease management. “From a cardiologist’s point of view, heart failure is the disease of the future, and we’re going to need a group approach to successfully manage it,” concluded Dr. Haddad.

