In April of this year, the University of Ottawa Heart Institute expanded its ranks with a new surgeon who brings broad interests in new concepts and technologies that have the potential to improve patient outcomes. Crossing the Atlantic from the Clinique Saint-Luc Bouge in Namur, Belgium, David Glineur, MD, PhD, is an internationally recognized specialist in two emerging areas of practice: robotic cardiac surgery and the use of an analytical tool, widely employed in cardiology, to improve cardiac bypass surgery.
Robotically Enhanced Cardiac Surgery
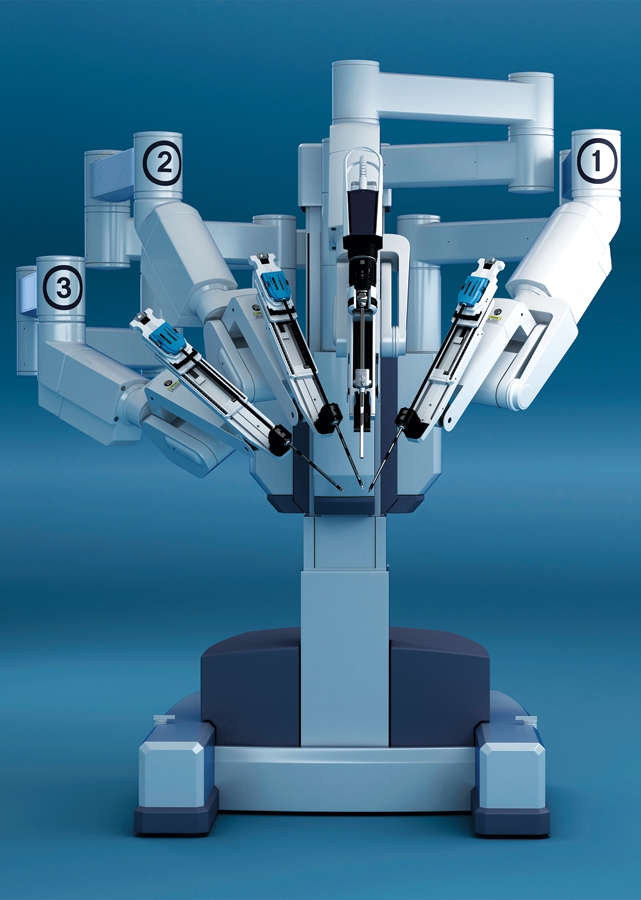
The use of robots for cardiac surgery has finally come into its own. After a rough start at the end of the 1990s, when the hype far exceeded the technology’s capabilities, there have been substantial advances in hardware and software. Now in its fourth generation, explained Dr. Glineur, robotic surgical equipment finally has truly transformative potential.
About five years ago, he saw evidence that the technology had matured, and he underwent intensive training in robotic surgery, with a focus on minimally invasive mitral valve repair.
“The major advantage with the robot is decreased surgical trauma,” he said. “You go from a complete sternotomy [open chest] to four small holes, each only about half a centimetre long. You are able to reconstruct the valve with the same quality as with open surgery, but the patient can return to his or her normal activity after three weeks.”
The current generation of robots offers smaller tools, 3-D visualization (which lets surgeons clearly see where they are in the heart), and a specialized arm for rotating and holding the heart motionless, in a manner similar to open heart surgery. With this capability, the robot can also be used to perform minimally invasive bypass procedures. The Heart Institute has been a pioneer in minimally invasive manual techniques.
While robotically enhanced surgery allows great precision with minimal trauma to the patient, the technique requires extensive training for surgeons to master the robotic interface and adapt to the lack of tactile feedback they rely on in manual procedures. Dr. Glineur underwent hundreds of hours of training before performing his first mitral valve repair with the robot.
“The robot is another excellent tool in our arsenal of options for the patient.”
– David Glineur, MD, PhD Cardiac surgeon, UOHI
Robotic surgery will not replace these manual procedures, he explained, because different surgical strategies are appropriate for different patients. “Robotic surgery is not for everybody; for example, it’s not for patients with valve calcification. But the robot is another excellent tool in our arsenal of options for the patient.”
The University of Ottawa Heart Institute Foundation has a campaign under way to raise the funds for the Heart Institute’s first surgical robot.
Lifting a Move from the Cardiology Playbook
Patients who are candidates for cardiac bypass surgery have one or more blockages in the arteries that supply blood to the heart muscle. Often these blockages don’t completely cut off blood flow. Fractional flow reserve (FFR) is a standard method for accurately measuring how much flow remains, but surgeons rarely use it.
“For 50 years, surgeons have been evaluating the severity of stenosis [blockage] by eyeballing,” said Dr. Glineur. “But fractional flow reserve is the only tool that can tell us, with high accuracy, the real severity of coronary stenosis.”
Widely used for a decade in interventional cardiology at the Heart Institute, FFR helps physicians determine whether an artery shown to be blocked on an angiogram actually requires stenting. It is measured using a tiny pressure sensor inserted into the blocked artery. The pressure is measured on both sides of the blockage and the ratio of these pressures indicates how much flow is still present. Although the angiogram provides a visual, what a blockage looks like is only an approximate measure of how much blood flow is restricted, explained Dr. Glineur.
Why do surgeons need to know the extent of a coronary blockage if they just plan to bypass it? The answer lies in the modern preference for using arteries instead of veins as bypass grafts, especially for patients younger than 70 at the time of surgery.
“If you put in a vein, one year after surgery, 20 per cent of the vein will be occluded. And after 10 years, 50 per cent will be occluded and 50 per cent will be very diseased. So after 10 years, if you use only veins for a bypass, the patient will have to undergo reintervention,” explained Dr. Glineur.
“Contrarily, if you use only arteries, after 10 years, only 10 per cent of patients need a new intervention. So, we try to place arterial grafts as much as possible, in order to decrease the reintervention rate in the long term,” he continued. Patients who receive arteries for their bypasses also have improved long-term survival.
The catch is that residual flow in a partially blocked artery can negatively impact the effectiveness of a grafted bypass artery. Veins are basically simple tubes. Blood flows through them without resistance. Arteries, on the other hand, are complex, responsive organs that expand and contract in order to help regulate blood pressure. Due to that responsiveness, when a healthy artery is grafted around a partial blockage, residual flow can compete and interfere with the flow through the graft as blood pulses with the heartbeat. This can compromise the delivery of blood to the heart muscle.
Dr. Glineur’s research has shown that surgeons can use FFR to determine where to place the grafted artery to minimize this competing flow. In some cases, FFR will indicate that a grafted artery would not be the best choice no matter where it’s placed, and a vein should be used instead.
“It’s a completely new concept in coronary surgery,” he said. “And I look forward to working in close collaboration with the interventional cardiology team here at the Heart Institute, which has international expertise in evaluating coronary stenosis.”

