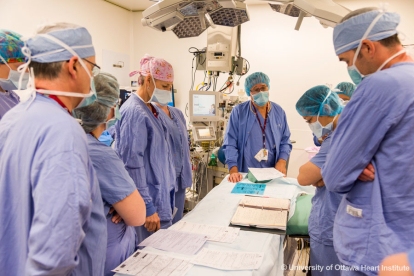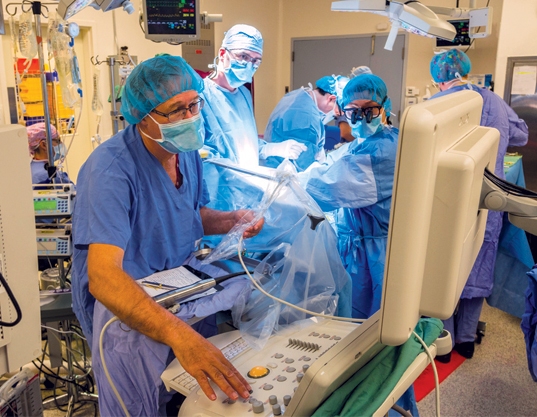
Cardiac procedures are a study in teamwork. Whether inserting a stent, implanting a pacemaker or performing corrective surgery, a team of professionals, each with a different set of skills, works in unison to achieve the best possible outcome for the patient.
“These are very much multidisciplinary teams. That’s what makes it so exciting and interesting,” said Dr. Donna Nicholson, a cardiac anesthesiologist at the University of Ottawa Heart Institute. Something that many people don’t realize, though, is that the role of the anesthesiologist on these teams can also be very much exciting and interesting. “The role of anesthesia is not well-known,” said Dr. Nicholson. “In fact, putting the patient to sleep is just the beginning.”
Drugs and Vitals
“We take care of the patient’s airway and ventilation, all of their lines, the echocardiogram, the IVs, drug support, all of the oxygenation and ventilation,” she continued. “We also handle blood volume replacement if there are complications. And, of course, we keep the patient asleep. We make sure patients don’t feel any pain, that they have no memory of the procedure.”
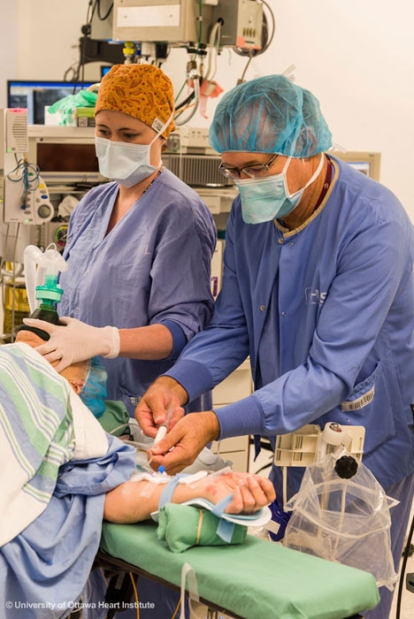
For a surgical procedure, such as cardiac bypass, there is about an hour of preparatory work before the surgeon makes the first incision. For the anesthesiologist, this involves administering a battery of drugs; inserting the various lines and IVs to deliver drugs, take measurements and insert catheters; and connecting the patient to the ventilator to assist breathing.
The drugs include standard ones for putting the patient to sleep and preventing pain—sedatives, analgesics, muscle relaxants—but go well beyond that. Antibiotics are given to avoid infection. If, after four hours, the patient’s chest is still open, a second dose is given. The anesthesiologist also manages coagulation of the patient’s blood. Heparin is given to prevent clotting during the surgery. Then, after the patient comes off the heart-lung bypass machine, protamine is given so that the blood will clot again.
All throughout the procedure, the anesthesiologist keeps the patient stable, fine-tuning the various drugs to keep the patient’s blood pressure within a target range. As Dr. Nicholson explained, “We manage the function and stability of the organ systems. While the cardiologists and surgeons are taking care of the procedure, we are keeping the patient alive.” It’s the anesthesiologist’s job to monitor the patient’s vital signs: blood pressure, heart rate, respiration, temperature, blood oxygen levels, cardiac output (blood flow) and pressures inside the heart.
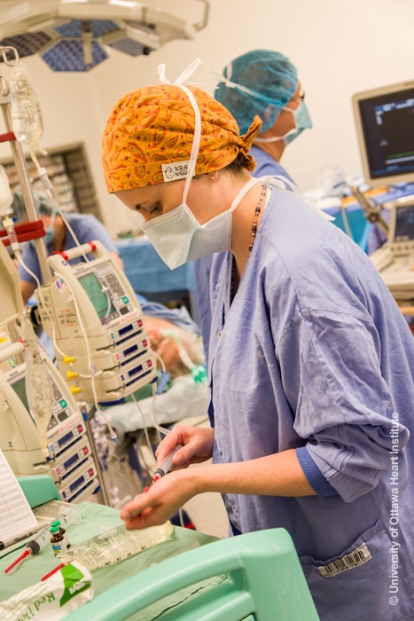
Because there is much else to do, they usually have a second pair of hands and eyes. “Respiratory therapists who have done additional training to work in the OR assist us with airway management, ventilation, blood product management, and mixing and organizing drugs,” she said. “For everything we do, they are our right hand.”
Getting the Inside Picture
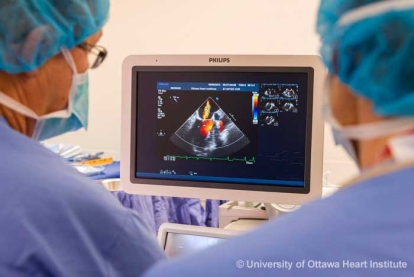
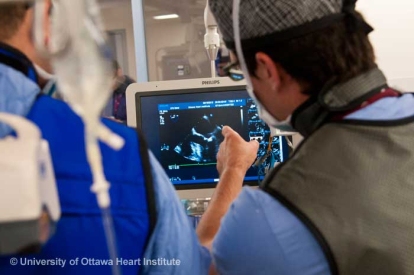
Thanks to some combination of angiogram, echocardiogram, computed tomography (CT) scan and possibly other imaging tests, the doctor performing the procedure has a good visual sense of what is happening with the patient’s heart beforehand. But the anesthesiologist provides real-time imaging during the procedure to see how the heart and valves are functioning then and there.
With transesophageal echocardiography (TEE) the anesthesiologist confirms what the cardiologist or surgeon has already seen. The TEE provides a standard visual assessment of the heart. Is there scar tissue present? Is there any leakage in the valves that wasn’t already known? This process identifies issues that could impact both the procedure and later recovery. If anything new or unexpected is found, the anesthesiologist passes this on to the rest of the team. He or she also takes visual measurements of the heart and calculates ejection fraction, which is a measure of how well the heart is functioning.
TEE is also used in a variety of other ways for particular procedures. For example, in bypass surgery, the anesthesiologist may use it to help the surgeon identify the best site for attaching a graft to avoid a location with plaque deposits.
For a non-surgical valve replacement known as a transcatheter aortic valve implantation (TAVI), TEE is central to the procedure. Before the new valve is implanted through a catheter, the anesthesiologist uses TEE to verify the size of the existing valve so that the implant fits properly. After the implant is inserted, TEE helps the team check the positioning and confirms that the implant is functioning as it should. The anesthesiologist also checks for any injury to the aorta. This capability to see and fix problems while the patient is still on the table significantly reduces the need to go back in to repeat or correct a procedure.
Specialized Roles
The anesthesiologist also plays specialized roles for certain procedures. At the moment that a TAVI implant is inserted, placement is critical. The contraction of the heart or the flow of blood could move the valve out of position. To bring everything briefly to a standstill, the anesthesiologist raises the patient’s heart rate to 160 beats per minute or more using an electrode called a pacing wire that is inserted into the heart through a catheter. This is called rapid pacing. At that rate, the heart is beating so fast that it no longer contracts and blood flow stops, allowing for precise placement of the new valve.
“While the cardiologists and surgeons are taking care of the procedure, we are keeping the patient alive.”
– Dr. Donna Nicholson, Cardiac Anesthesiologist, UOHI
Another example is deep hypothermic circulatory arrest. “For some surgical procedures, we put the patient on cardiopulmonary bypass, cool them to 18 to 20 degrees Celsius and then stop the pump,” explained Dr. Nicholson. “At that point, the patient has no vital signs. This cooling protects the brain.” This state can last 30 to 60 minutes or longer, with additional techniques.
“We work closely with the perfusionist [the heart-lung bypass expert] on this,” she continued. “We take care of temperature management, metabolic control, drug therapy. We manage complications that may occur after the circulatory arrest. We work on coagulation of the blood, replacing platelets, plasma, red blood cells.”
Perioperative Care
As the procedure is wrapping up, the anesthesiologist enters data into the perioperative database. With more than 30,000 patient records, the Heart Institute’s archive is one of the largest such databases in the world and a long-standing project for the Division of Cardiac Anesthesiology. The physicians in the division mine this remarkable collection of information, conducting research to improve patient care and outcomes. One current study examines complications following surgery.
The anesthesiologist then fills out a checklist to identify any particular concerns or problems anticipated in recovery.
“When the team carrying out the procedure is finished, we’re still caring for the patient—waking the patient up, transferring him or her in a stable condition to the Cardiac Surgery Intensive Care Unit [CSICU], which is run by our division,” said Dr. Nicholson. “We consider ourselves perioperative physicians. We do preoperative, operative and post-operative care.”
“We have a unique environment here at the Heart Institute,” she concluded, “Our CSICU is run by cardiac anesthesiologists, ensuring continuity of care from the procedure through recovery. There really is no other heart facility like ours in Canada.”