Editor’s Note:
In this issue, The Beat continues with Part 2 of “The Changing Cardiovascular Patient”, in which we look at trends and changes in cardiovascular medicine. First, we examine the challenges of cardiovascular care posed by the aging Canadian population and the corresponding rise in people living with related chronic conditions. As well, we look at the changing face of cardiovascular medicine in our story “The Revolution in Cardiovascular Care.” We have talked about the current state of cardiovascular care. Now, we sit down with two of the Heart Institute’s leading cardiologists and examine the evolution in cardiac care over the last 50 years.

Treating chronic disease is one of the most common and costly challenges facing Canada—and much of the developed world—today. Major conditions, such as cardiovascular disease, diabetes and arthritis, for example, have similar risk factors and links to specific behaviours. Physical inactivity, excess weight, tobacco use, and unhealthy diet are lifestyle issues that rely significantly on patient action to manage with direction and support from allied health care staff.
Together, cardiovascular patients with physicians, nurses, educators, physiotherapists and an ever-growing health care team are part of an alliance making a significant investment in managing one of the most serious chronic conditions—cardiovascular disease.
The Government of Ontario’s framework to encourage informed decision making and discussion about chronic disease clearly explains how patients and families need to play an important, active role. That means patients developing solid partnerships with their health care providers by participating in planning and self-managing their conditions.
Taxing the System
“If everything falls as predicted, the aging population is going to be a perfect storm for all of health care, but it’s going to be particularly difficult for cardiovascular disease,” said Dr. Lyall Higginson, cardiologist and former Chief of Cardiology at the Heart Institute and past President of the Canadian Cardiovascular Society. “As we’re dealing with acute disease more effectively, people are living longer, and they’re living with a multiplicity of chronic conditions that we have to deal with in new and different ways.”
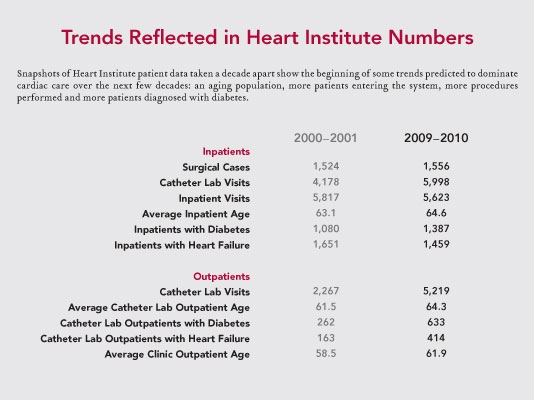
“This upcoming wave of patients living with chronic diseases (see table below) threatens to overload Canada’s already impacted hospitals,” Dr. Higginson said. “We need to improve chronic care outside the hospital; for example, nursing homes need to grow their ability to look after medical problems so we can move people through the hospital faster,” he continued.
Physicians will also need to become more familiar with chronic disease management and working in multidisciplinary teams in order to take care of patients with a myriad of health problems. “People with multiple chronic diseases are going to need an incredible ‘quarterback’—one person who is in charge of their care in all the areas of concern. I think we’re going to need a new training mechanism for our family physicians, who will have to be very comfortable in this role,” he said. Greater involvement from special practitioners, such as advanced practice nurses or physician assistants, will also likely be required due to the over-whelming number of patients predicted to be entering the system with conditions that will need lifetime management.
Continuity of Care
A greater role for community hospitals in providing cardiac care will also be needed, predicted Sharon Ann Kearns, manager of Quality and Risk for the Heart Institute. Her team recently developed several sets of guidelines and care plans for patients with acute coronary syndrome and heart failure, for use not just at the Heart Institute but among its regional partners as well.
“We’re partnering more with our patients, educating them more and asking them more for help regarding their own care.” – Dr. Lyall Higginson, Cardiologist and Former Chief of Cardiology, UOHI

“We’ve developed these tools here at the Institute and rolled them out across all of our referring hospitals so that patient care is managed the same way there as it is here,” she explained. One of the most important of these has been the Guidelines Applied in Practice (GAP) tool, a discharge checklist and a patient education resource that is sent home with each patient after discharge from the Heart Institute.
In addition to capturing the care received at the Heart Institute and medications taken, the GAP tool carries data to the primary care physician about additional medications to start during recovery. The tool also delivers information to the patient and family about needed lifestyle changes, such as rehabilitation and smoking cessation. “We’re trying to ensure that at transition points, everyone is getting all the appropriate information they need and that they understand who is responsible for the different aspects of their care,” she continued.
The Heart Institute is currently partnering with the Canadian Institute of Health Information (CIHI) to capture the GAP tool information in the CIHI database in an effort to make the care plan portable across Canada.
Helping Patients Help Themselves
Providing patients with an understandable, comprehensive summary of their treatment is just one step in helping patients become better partners in their own care. “I think a huge advance in the last 10 or 15 years has been the concept of self-management. More and more, patients are understanding their multiple problems and taking control of their diabetes, their high blood pressure and so on,” said Dr. Higginson. “We’re partnering more with our patients, educating them more and asking them more for help regarding their own care.”
An example of this partnership is the telehome monitoring program, in which patients are trained to take many of their own measurements, such as body weight, fluid intake, blood pressure and blood glucose levels. These measurements are then transmitted from the patient’s home to a Heart Institute nurse who evaluates whether an adjustment to medications or a clinic visit is in order.

In the coming decade and beyond, the Heart Institute will be rolling out extensive education and rehabilitation programs to help physicians care for patients with heart disease in their own communities and to better empower patients to play a greater role in their own care.
One of the things that makes people better self-managers, said Jane Brownrigg, the Heart Institute’s Program Director for Cardiac Rehabilitation outreach programs “is helping people understand why: why we have particular recommendations around physical activity or stress management or medication compliance, for example.”
The time in hospital immediately after a heart attack or other acute event is not always the best time to learn that information, she continued. “When I was working as a bedside nurse, I distinctly remember how many patients were just reeling from the fact that they’d had a heart attack at the same time that they had an awful lot of information coming their way.”
To provide education when patients have the time, energy and ability to focus on new information, the Heart Institute has recently begun implementing several programs designed to help them manage heart disease as a chronic condition. Some have been developed and evaluated elsewhere, while others are initiated and assessed at the Heart Institute. One is a course called “Living a Healthy Life with Chronic Conditions.” Developed at Stanford University in Palo Alto, California, it teaches patients health management and goal-setting skills and is open to families and caregivers in addition to patients.
Other new programs include a course teaching patients about medication compliance; FrancoForme, a phone-coaching program targeting French-speaking patients with risk factors for heart disease; and CardioFit, a web-based exercise program for patients not participating in traditional cardiac rehabilitation.
“We’re really looking to increase access to services that help people with cardio-vascular disease management and save them from coming to us physically whenever possible. Nobody wants to be hospitalized if they can avoid it,” said Brownrigg.
Providing Comfort and Facing the Future
Another aspect of disease management likely to play a larger role in the future of cardiovascular medicine is palliative care. Often confused with end-of-life care, palliative care is any type of care that provides comfort and symptom relief to patients during their illnesses. For patients with chronic heart disease, this can mean for the rest of their lives.
“Previously, patients with acute heart disease tended to die quickly, so palliative care for heart disease just wasn’t on anyone’s radar. Now, care has improved and patients are living longer, and we need to provide comfort measures to them,” explained Kearns.
The Heart Institute has begun to work with the University of Ottawa’s palliative care team over the past few years, she said, particularly in the care of patients with pulmonary hypertension and end-stage heart failure.
All of these initiatives and more will be required to help the health care system manage the changing cardiovascular patient. “As patients who survive a heart attack get older, we’re going to have more and more cases of chronic heart failure to deal with. Ongoing management of diabetes and coronary artery disease are also going to be major challenges as we go on. And obesity is a huge problem in Canada, and we don’t have any magic solutions in that area,” said Dr. Higginson. “We’ve got to continue to be innovative in order to handle the growing burden of disease,” he concluded.

