The heart is a muscle that works like a pump. The main job of the heart is to pump blood throughout the body. Cardiomyopathy is a condition which affects the ability of the heart muscle to pump effectively. There are different types of cardiomyopathy and different causes. The main goal of treatment is to reduce symptoms – cardiomyopathy is not curable. Most types of cardiomyopathy are treated with medications and lifestyle changes. In some cases, there are surgical options which may help to reduce symptoms and protect you from life-threatening abnormal heart rhythms.
Types of Cardiomyopathy
Cardiomyopathy is a disease of the heart muscle. There are several different types of cardiomyopathy.
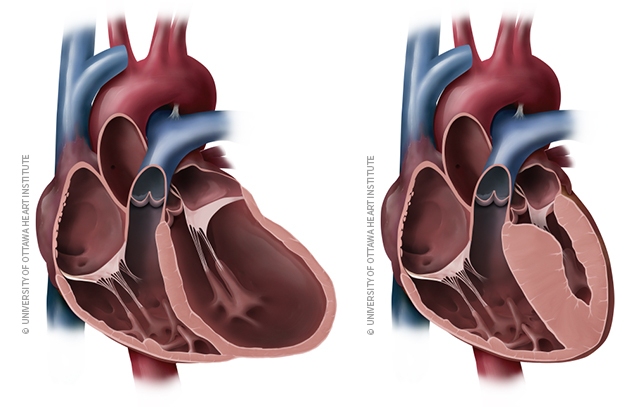
Dilated Cardiomyopathy
This is the most common type of cardiomyopathy. One or more chambers of the heart become enlarged, and the muscles that make up the walls of the heart become stretched and thinner than normal. This stretching further weakens the muscles, and the heart is not able to pump blood as strongly.
Hypertrophic Cardiomyopathy
Muscles in the heart become abnormally thickened, and the heart has to work harder to push the same amount of blood through the body. In obstructive hypertrophic cardiomyopathy, the thickened muscles push into a chamber of the heart, blocking blood flow and sometimes causing the mitral valve of the heart to leak.
Restrictive Cardiomyopathy
In this rare type, the heart muscles become stiff, and the ventricles of the heart are not able to relax and completely fill with blood between heartbeats.
Arrhythmogenic Right Ventricular Cardiomyopathy
Heart muscle cells are replaced by scar tissue or fat, leading to disturbances in the electrical signalling of the heart. These disturbances can cause sudden cardiac death.
All types of cardiomyopathy can lead to abnormal heart rhythms (arrhythmias), blood clots, heart attack, or heart failure.
On this page
Causes
There are many causes of cardiomyopathy. Some types are inherited. They are caused by genetic conditions passed from parents to their children. In addition, many other medical conditions can cause cardiomyopathy, including:
- Congenital heart disease
- Coronary artery disease
- Chronic high blood pressure
- Previous heart attack, causing damage to the heart muscle (called ischemic cardiomyopathy)
- Heart valve disease
- Viral or bacterial infections of the heart
- Excessive alcohol consumption
- Use of cocaine or other street drugs
- Treatment with some types of chemotherapy or radiation therapy for cancer
- Diabetes and other metabolic diseases or disorders
- Some nutritional deficiencies
- Complications from pregnancy
Cases in which the cause cannot be determined are known as idiopathic cardiomyopathies. The cause of cardiomyopathy does not need to be known for a patient to undergo treatment.
Diagnosis
Tests commonly used to diagnose cardiomyopathy include:
- Echocardiogram: to determine the volume of blood pumped by the heart
- Electrocardiogram: to identify problems with heart rhythm
- Chest X-rays: to look at the size and shape of the heart
- Holter monitor: to continuously monitor the heartbeat over one or two days
- Cardiac catheterization: to identify blocked or restricted blood vessels and take tissue samples (biopsies) if needed
- Stress (exercise) testing: to measure how well the heart functions when challenged to work harder than normal
- Blood tests
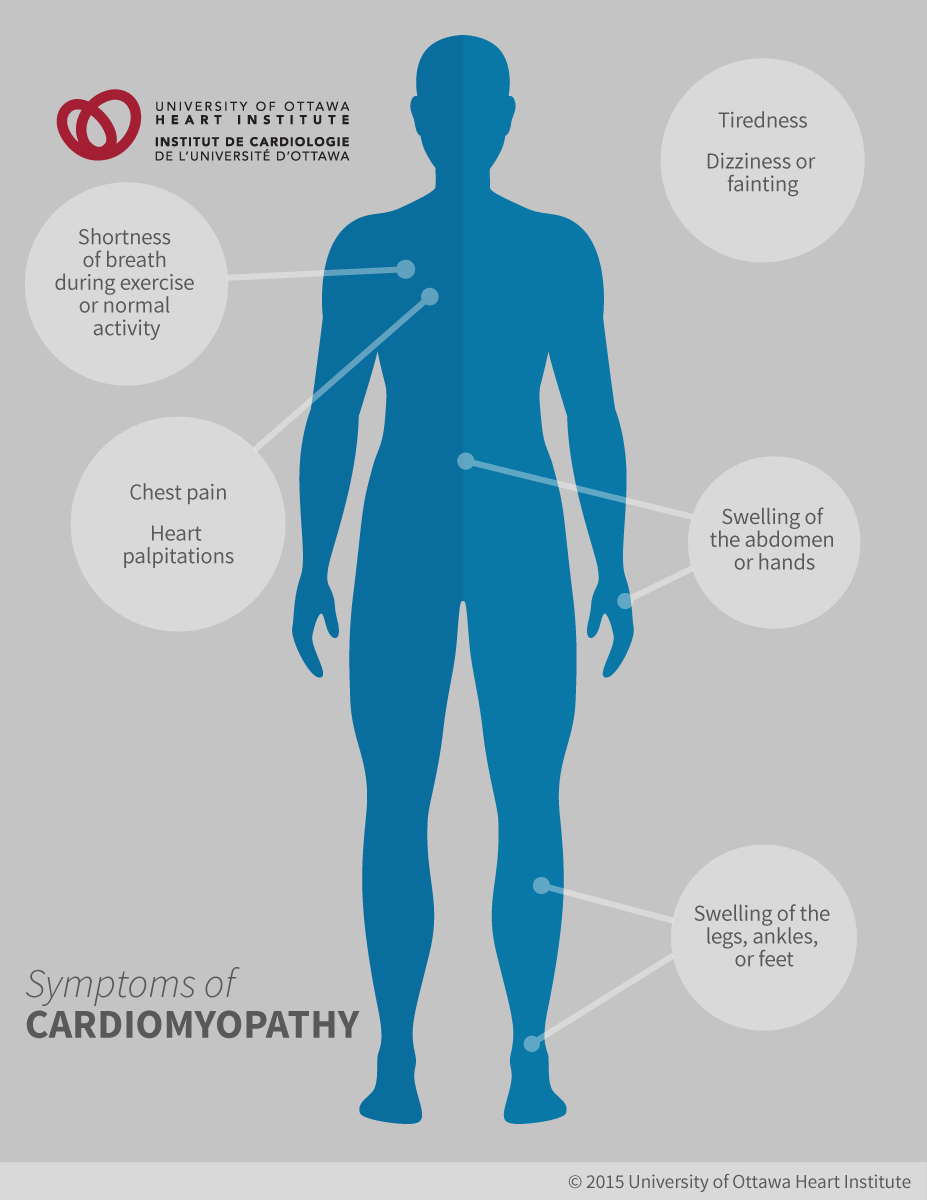
Symptoms
Cardiomyopathy may not cause symptoms in its early stages. As the disease gets worse, symptoms can include:
- Shortness of breath, during exercise or normal activity
- Dizziness or fainting
- Chest pain (angina)
- Tiredness
- Abnormal heart rhythms
- Heart palpitations (a racing or irregular heartbeat)
- Swelling in the hands, legs, ankles, feet, or abdomen
Many of these symptoms can be confused with the effects of aging or physical inactivity, or with other diseases affecting the heart or lungs.
Treatments
Cardiomyopathy is treated with lifestyle changes, medications, implantable devices, special cardiac procedures, or surgery. Many treatments can be used for more than one type of cardiomyopathy. Only a trained specialist can determine the appropriate methods for any particular case.
Lifestyle Changes
People with any type of cardiomyopathy can benefit from the following:
- Reducing salt in the diet helps lower blood pressure. If a patient is overweight, losing weight can help relieve the symptoms of cardiomyopathy by reducing the burden on the heart.
- Limited or no alcohol consumption is recommended for people with cardiomyopathy, as alcohol can depress the functioning of the heart.
- Light or moderate exercise to improve cardiovascular fitness can be beneficial for some people with cardiomyopathy. Because of the potential risk of sudden cardiac death, patients should speak with their doctors before beginning an exercise program.
Medications
Many medications are available for reducing the symptoms of cardiomyopathy. These include drugs to:
- Lower blood pressure (ACE inhibitors or angiotensin receptor blockers)
- Slow the heartbeat (beta blockers)
- Help relax the blood vessels (calcium channel blockers)
- Keep the heart rhythm normal (antiarrhythmic drugs)
- Dilate (open) the blood vessels
- Help prevent blood clots (anticoagulants (blood thinners), such as warfarin)
- Remove excess fluid in the body (diuretics)
- Help the heart pump more blood (digoxin, also known as digitalis)
Implantable Devices
Some people with cardiomyopathy may need a device implanted in their chests to help the heart work properly.
- A biventricular pacemaker can help coordinate the activity of the left and right sides of the heart.
- An implantable cardioverter-defibrillator (ICD) can monitor heart activity and deliver a small electrical shock to restore normal heart rhythms when needed. An ICD may be implanted in patients deemed at high risk for sudden cardiac death due to cardiomyopathy.
Non-surgical Procedures
Some patients with obstructive hypertrophic cardiomyopathy may undergo a procedure called alcohol ablation, in which alcohol is injected through a small artery into the heart to remove excess heart tissue blocking the blood vessels.
Surgery
Some patients with cardiomyopathy may need surgery if their disease cannot be controlled with less invasive treatments.
In a procedure called septal myotomy-myectomy, performed in patients with obstructive hypertrophic cardiomyopathy, the doctor surgically removes a piece of the thickened heart muscle that is blocking blood flow through the heart. A poorly functioning mitral valve can be repaired or replaced at the same time.
Rarely, a patient with life-threatening cardiomyopathy may receive a heart transplant. This procedure can only be done in patients who are healthy enough to undergo major surgery. Patients waiting for a transplant may have a left ventricular assist device (LVAD) implanted. LVADs are artificial pumps that can help the heart pump blood when the heart is too weak to function on its own.