Heart failure is a condition in which the heart does not pump as strongly as it needs to. When the heart is not pumping well, the rest of your body does not get enough blood and oxygen. Heart failure is the most common diagnosis that brings people to the hospital for admission. Many new cases are diagnosed each year.
The heart is a muscle that works like a pump. Its main job is to pump blood throughout your body. Heart failure occurs when your heart is no longer strong enough to provide your body with all the blood and oxygen it needs. This happens because your heart has become damaged or weakened. When this occurs, your heart works harder than normal and less efficiently. This increased effort can cause physical changes in the heart over time. These changes can include enlargement of the heart and thickening of the ventricle walls.
Heart failure does not mean that your heart will suddenly stop working or that you are about to die. It means that your heart has to work too hard to keep the blood flowing to the rest of your body.

Heart Team
Heart failure is a complex condition which can progress without careful monitoring and management. At the Heart Institute, our Heart Failure Heart Team brings together experts from many disciplines for a holistic approach in guiding the care of each individual patient.
The Heart Failure Heart Team includes cardiologists, surgeons, anesthesiologists, nurses, nutritionists, rehabilitation specialists and other allied health professionals.
On this page
Causes
The most common cause of heart failure is a heart attack that caused damage to some of your heart muscle. If a lot of heart muscle is damaged from a heart attack, the heart becomes weak and heart failure may occur. Heart failure is not the same as a heart attack.
Another key cause is long-term high blood pressure (hypertension) that has been not well controlled.
Some additional causes of heart failure include:
- Hypertrophy. This is a stiffening of the heart muscle which leads to the heart muscle becoming thickened. It is commonly seen in the elderly.
- Cardiomyopathy (from Greek: cardio means heart and myopathy means muscle abnormality). This is a heart muscle problem which can be due to a virus, a history of high alcohol consumption, or an unknown cause.
- A heart valve abnormality
- Abnormal heart rhythms (arrhythmias)
Diagnosis
Many symptoms of heart failure can be easily confused with the effects of aging or physical inactivity. Your doctor will start by reviewing your medical history with you, and will conduct a full physical exam. Doctors often order a number of tests to determine if you have heart failure. These include:
- Chest X-ray: to look at the size of your heart and help determine whether there is fluid in your lungs
- Electrocardiogram (ECG): to look at your heart rhythm
- Blood tests: to determine various things including your kidney function.
- Echocardiogram and/or heart scan (MUGA scan): to look at the overall structure of the heart chambers and valves and to determine your ejection fraction.
Ejection fraction (EF) is a measure of how well your heart is pumping. People with a healthy heart usually have an ejection fraction of 50% or greater. Many people with heart failure have an ejection fraction of 40% or less. However, it is possible to have heart failure with a normal EF.
Symptoms
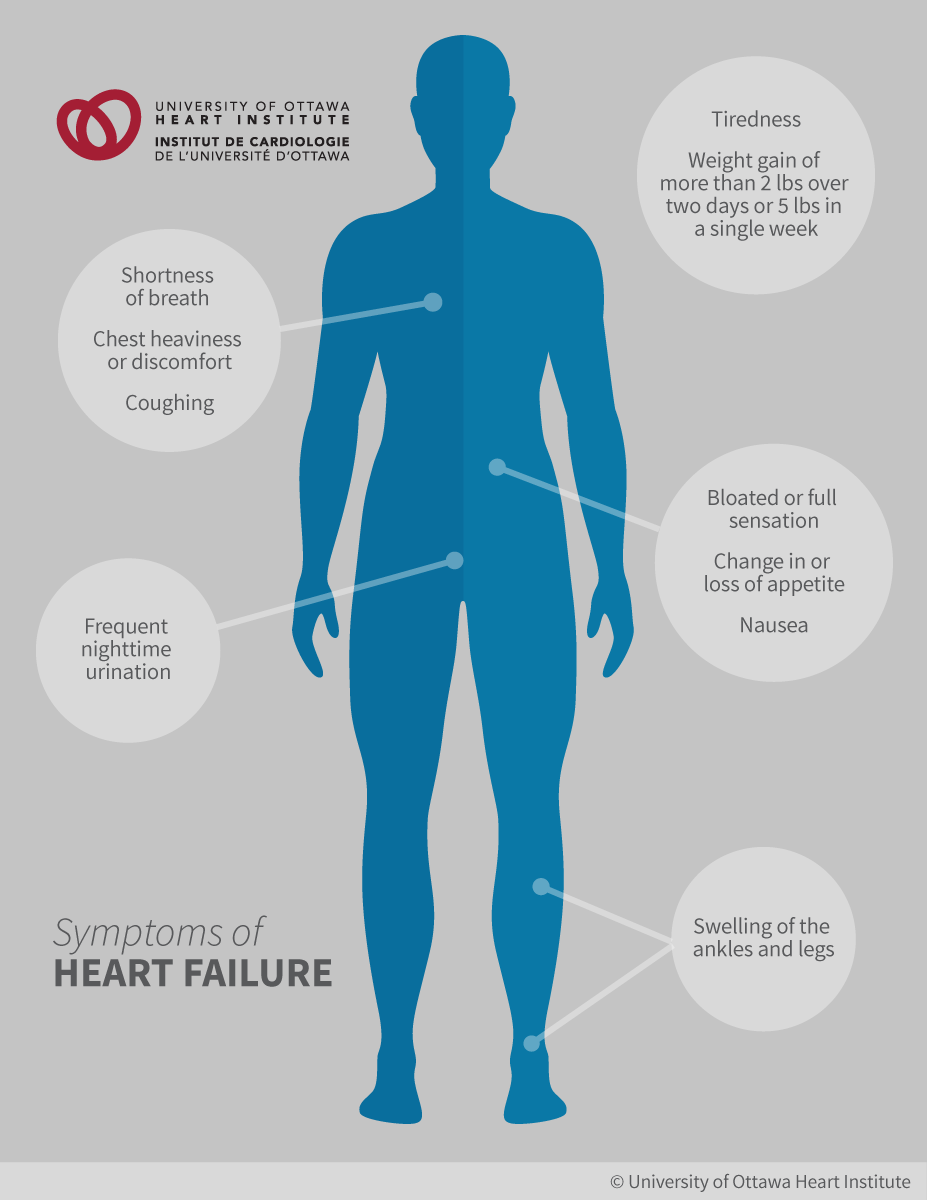
Common symptoms of heart failure include:
- Feelings of tiredness and weakness
- Shortness of breath, which can happen even during mild activity or at night during your sleep
- Difficulty breathing while lying down flat
- Weight gain from fluid retention
- Swelling in the legs, ankles or stomach area
Treatments
There are many treatment options for heart failure. Additional options become available with new research.
Medications
Certain types of medications help prevent future heart failure episodes and may help you live a longer and healthier life. Each medication helps in a different way. (A description of heart failure medications can be found in the Heart Failure Patient Guide).
The medications your doctor prescribes are tailored according to your particular condition and type of heart failure. It is common to have medication and dosage changes during your initial treatment and follow-up appointments.
Lifestyle Changes
Changes in diet, weight loss, and physical activity help alleviate symptoms and improve prognosis. In particular, fluid restrictions and a low-salt diet are essential.
Smoking, high blood pressure, and excess weight all increase the risk of developing heart failure and related conditions. Each of these risk factors can be controlled to help prevent the onset of heart failure and other forms of heart disease.
Surgery
Surgery may be an option for some types of heart failure.
- Implantable cardiac defibrillator (ICD) or cardiac resynchronization therapy (CRT)
- Coronary artery bypass graft
- Valve repair or replacement
Telehome Monitoring
Our Telehome Monitoring program can help heart failure patients stay on track with their medications, fluid and dietary restrictions, and physical activity. The program uses a combination of automated telephone assessments and remote collection of patient vital signs.
Patient Education
Patients who play an active role in the ongoing management of their heart failure are better able to keep the condition under control, slow its progress and reduce the likelihood of being readmitted to the hospital. This makes learning about your condition and what you can do to help manage it an important part of treatment.
Our Heart Failure Patient Guide and related videos provide tools and information to help you and your loved ones manage your heart failure
Resources
- Heart Failure Patient Guide
- Heart Failure Cardiac Rehabilitation Virtual Education Series (video series, Youtube)
- Heart Function Clinic
- UOHI Webinar Series: Heart Failure Discharge Class for Patients and Families
- Canadian Heart Failure Network