Atrial fibrillation is a type of irregular heartbeat, or arrhythmia, that happens when the electrical signalling in your heart is disrupted. Different types of atrial fibrillation may last for seconds or be permanent. The condition is more common in older people and can have many different causes.
Many people who have atrial fibrillation lead perfectly normal lives, but having atrial fibrillation does increase your risk for stroke.
About Atrial Fibrillation
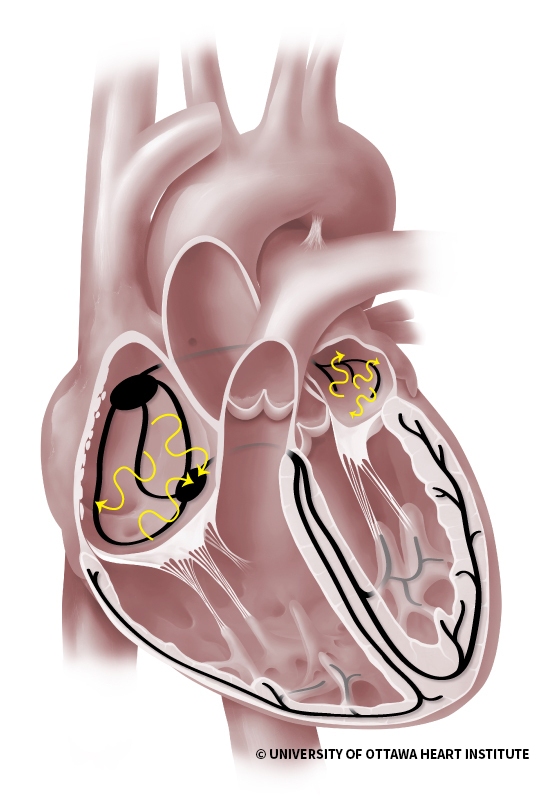
Normally, the pumping of your heart is regulated by an electrical current or impulse—much like a spark plug in a car. The electrical impulse starts in the sinoatrial (SA) node and then spreads throughout both atria like ripples in a pond. This causes both atria to contract, squeezing blood into the ventricles.
The impulse then travels down to the atrioventricular (AV) node which is like a wire that connects it to the ventricles. The AV node splits into two branches, allowing the even spread of the electrical signal to both ventricles at the same time. Both ventricles then contract to squeeze the blood out to your body.
When the heart is working properly, this cycle repeats 50 to 150 times per minute.
In atrial fibrillation, the electrical impulses start firing from all over both atria in an irregular pattern. With too many random triggers firing, your heart beats irregularly and, sometimes, too fast.
Atrial Fibrillation and Your Heart Video Series
This series for patients and caregivers provides information about the care and management of atrial fibrillation.
There are different types of atrial fibrillation:
Paroxysmal
You have bouts of atrial fibrillation that come and go. They may last a few seconds or up to several days, but usually, they start and stop on their own.
Persistent
Your episodes of atrial fibrillation last longer than a week and, usually, won’t stop without some kind of treatment.
Permanent
Your heart is always in atrial fibrillation. Your doctor may have tried several different types of treatments, but nothing has returned your heart to a normal rhythm. It is unlikely your heart will ever go back to a normal rhythm.
Many people who have atrial fibrillation lead perfectly normal lives.
Atrial Flutter
Atrial flutter is similar to atrial fibrillation but less common. Many patients have both atrial flutter and fibrillation. They are very closely related. In fact, the treatments for both are similar and the risk of stroke from both is the same.
On this page
Causes

Atrial fibrillation is a common condition in older adults. In fact, according to the Heart and Stroke Foundation, about one of every 10 people older than the age of 80 has atrial fibrillation.
Different types of heart conditions such as heart valve disease, heart attack or heart failure, can cause atrial fibrillation. Any type of infection that causes inflammation of the heart muscle or the outer layer of the heart may lead to atrial fibrillation. Some people who are born with heart problems may develop atrial fibrillation later in life.
Other health conditions such as high blood pressure, diabetes, sleep apnea, or lung disease may also increase the risk of developing atrial fibrillation. In many cases, people develop atrial fibrillation for reasons that are not known.
Possible Complications of Atrial Fibrillation
Left untreated, atrial fibrillation puts you at risk for serious problems such as stroke or heart failure.
Stroke
Because your atria cannot move blood properly, your blood starts to pool and get stuck in the small corners and grooves of the heart. Once stuck, the blood can start to clot. With all the irregular contractions in your atria, these clots can break free and get pumped into the circulation.
If a clot reaches the brain, it can get lodged in one of the blood vessels and cut off the blood supply to that part of the brain. This is a stroke. Rarely, these clots can also go to other parts of your body and cause other complications.
Heart Failure
If atrial fibrillation is not controlled, your heart can become weaker and you may develop heart failure. This occurs when your heart has to work too hard to keep blood flowing throughout your body. As a result, extra fluid builds up. This fluid retention can cause swelling of your ankles and lower legs, or it can build up in your lungs resulting in breathing difficulties and extreme fatigue.
Other Complications
For some people, atrial fibrillation can cause great tiredness, weakness, or breathing problems. Uncontrolled atrial fibrillation can also cause chest pain, dizziness, and extreme fatigue. In the elderly, it can cause bouts of confusion. Although not life threatening, these symptoms can limit your everyday activities and lower your quality of life.
Diagnosis
Often, atrial fibrillation is diagnosed when people develop symptoms and go to their doctors or to the emergency department. Other times, it is picked up during routine examinations. In order to diagnose atrial fibrillation, your doctor will review your medical history, conduct a full physical exam and order some tests.
Some of the more common tests your doctor may order include:
- Electrocardiogram (ECG): This test records the electrical activity of your heart and is important for confirming whether your heart rhythm is in atrial fibrillation
- Holter Monitor: This test is like an ECG except that it records your heart’s electrical activity for up to 48 hours. It requires you to be connected to a small portable device which is carried with you for two days in a pouch or on a shoulder strap. The Holter monitor is helpful if you have only occasional bouts of atrial fibrillation that do not show up on an ECG.
- Event Recorder: Similar to the Holter monitor, the event recorder is a device you wear for up to two weeks. You press the “record” button whenever you experience anything you think is abnormal, such as rapid heartbeats, dizziness or chest pain. These recorders may also pick up episodes automatically.
- Echocardiogram: This is a special ultrasound test for the heart that lets your doctor have a closer look at the chambers and valves in your heart.
Symptoms
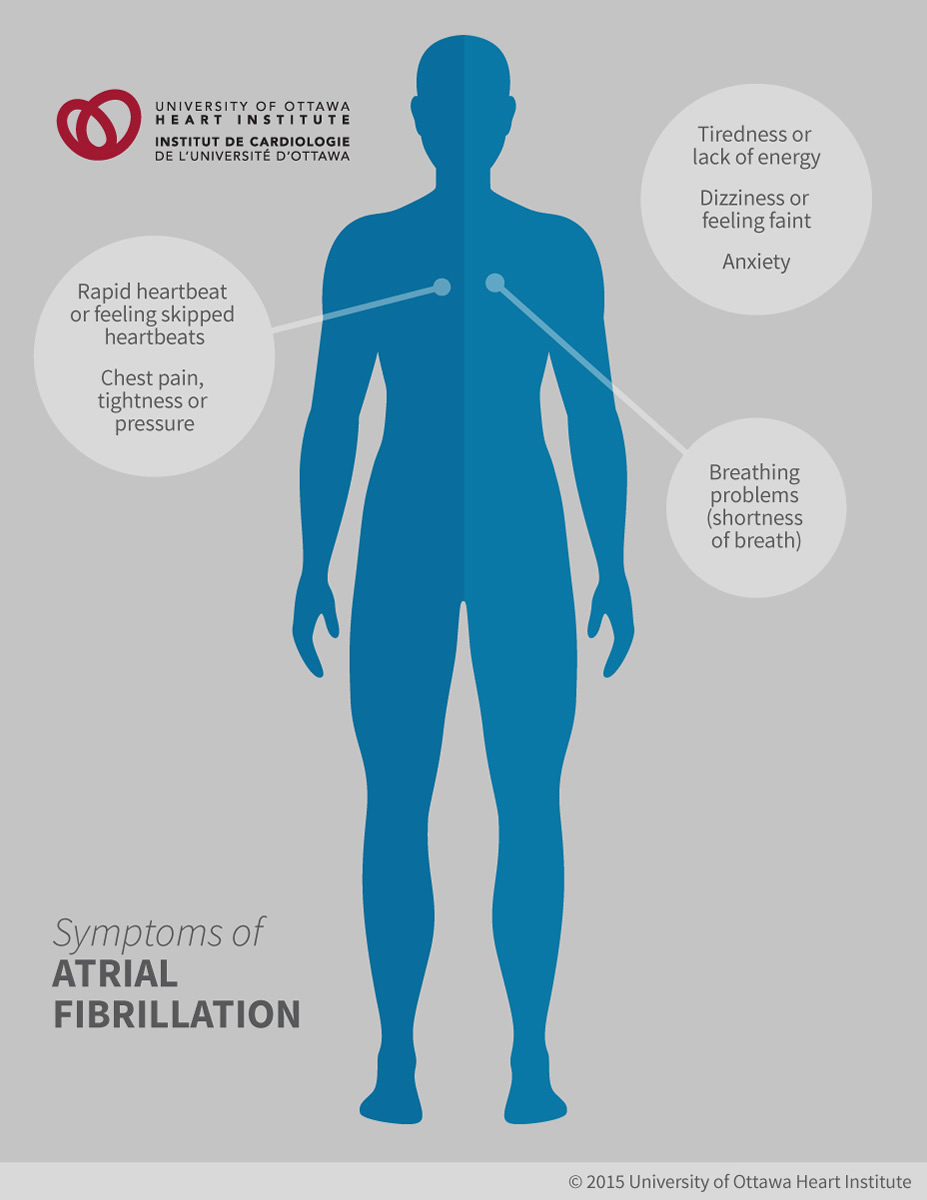
Atrial fibrillation can cause you to feel any of the following symptoms:
- Rapid heartbeat or feeling “skipped” heartbeats
- Breathing problems (shortness of breath)
- Dizziness or feeling faint
- Tiredness or lack of energy
- Chest pain, tightness or pressure
- Anxiety or feeling like something is not quite right
These are the most common symptoms. You may feel only one or two or you may have different symptoms. Many people have no symptoms at all. In fact, many people with atrial fibrillation are able to keep their symptoms at a minimum and have an excellent quality of life.
Click to enlarge
Treatments
By itself, atrial fibrillation is usually not a life threatening condition, but it still must be treated because:
- Atrial fibrillation can impact your quality of life and prevent you from doing the things you normally do.
- Atrial fibrillation slows down the regular flow of blood through the heart, increasing the chances that the blood will pool and form clots. If a clot is pumped out of the heart, it can lead to a stroke.
Reducing Symptoms with Medications
There are two main approaches to treating your symptoms: rate control, to slow your heart to a more normal rate, and rhythm control, to restore a more regular heart rhythm. The choice of treatment plan will depend on a number of factors, including:
- The type of atrial fibrillation you have
- Your other heart conditions or health issues
- Your symptoms
- Your preferences
Many patients start with one medication but may need to have it changed as their conditions progress.
Reducing Your Risk of Stroke with Anticoagulant Medications
To prevent blood from clotting inside your heart, your doctor may put you on a medication called an anticoagulant—sometimes called a blood thinner. Anticoagulants don’t actually thin your blood. Rather they increase the time it takes to form a blood clot. The type of anticoagulant your doctor recommends for you will depend on other medical conditions you may have, along with your overall risk of stroke.
Anticoagulants are very effective at reducing your risk of stroke and are recommended for almost all people who have atrial fibrillation. Some anticoagulants require regular blood tests when first taking them until the best dose is determined.
Procedures
The most common procedures for treating atrial fibrillation are electrical cardioversion and catheter ablation.
- Electrical Cardioversion: This procedure involves delivering a shock to your heart much like a defibrillator would only with a smaller amount of electricity. If you are scheduled to have a cardioversion, you will come in to the Heart Institute for the day. You will be given a medication to help you sleep and relax. Once this medication has taken effect, the defibrillator pads will be placed on your chest and a small shock will be delivered. You will not remember the shock and you will not feel any pain. After the procedure, your doctor may start you on a rhythm control medication to help your heart to stay in normal rhythm.
Cardioversion is only a short term solution. In most patients, the atrial fibrillation comes back.
- Catheter Ablation: This procedure involves inserting thin wires through the veins in your groin or neck. The tip of the ablation catheter is directed toward the areas in your heart that are firing off the irregular impulses. Once properly positioned, the catheter delivers a small radiofrequency electrical current to burn out the tiny areas.
- Other Treatments: In some situations, your doctor may recommend that you have a pacemaker implant or surgery called a maze procedure to treat your atrial fibrillation.
Resources
- Atrial Fibrillation Patient Guide
- Research Study: Atrial Fibrillation
- Heart and Stroke Foundation’s Atrial Fibrillation Guide
- American Heart Association’s Afib Town
- St. Michael's Hospital's Atrial Fibrillation Video Series

