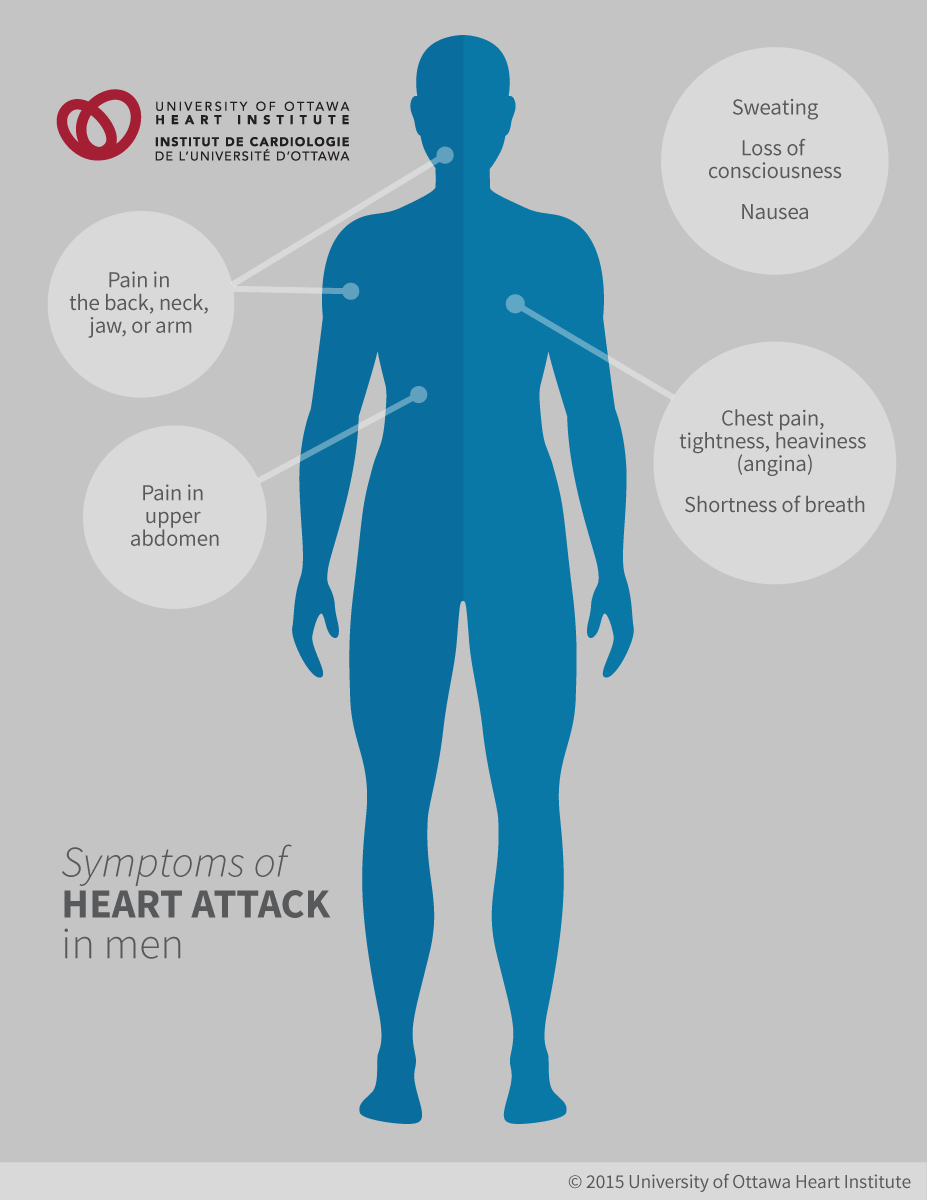
A heart attack happens when the supply of oxygen-rich blood is cut off from part of the heart muscle. Heart attacks are usually caused by blockages in the arteries that provide the heart with blood. People having a heart attack will often experience chest pain or tightness, pain in the back, neck, jaw, or arm, shortness of breath, sweating, nausea, or, sometimes, loss of consciousness. The immediate treatment for a heart attack is to find the blocked arteries and open them up. Ongoing care that includes lifestyle changes and new medications is also required to ensure the best recovery possible.
What Is a Heart Attack?
On this page
Causes
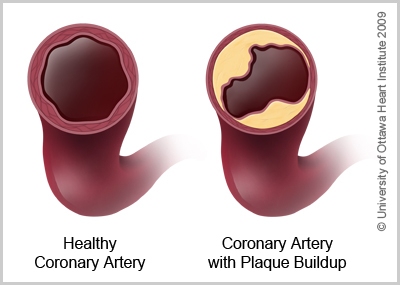
The most common cause of heart attack is coronary artery disease – or narrowing of the coronary arteries -- the blood vessels which supply the heart muscle with oxygen-rich blood. The narrowing of these arteries is usually caused by the buildup of cholesterol plaque in the artery walls. This buildup is called atherosclerosis or hardening of the arteries.
Sometimes, the plaque in the artery can crack open. When this happens, the blood flowing past can form a clot, reducing or blocking the supply of blood. This loss of blood supply to the heart muscle can cause the cells to die.
There are two types of heart attack:
ST-Elevation Myocardial Infarction (STEMI)
If the coronary artery in question gets completely blocked, blood flow stops entirely and the full thickness of heart muscle fed by that artery is damaged. This causes a characteristic change on the electrocardiogram (ECG) readout called an ST-segment elevation.
Non-STEMI Heart Attack
If the coronary artery is only partially blocked by clots, blood flow decreases but does not stop. Only part of the heart muscle is damaged and ST-segment elevation is not seen on the ECG. This is called a non-ST-elevation myocardial infarction or non-STEMI heart attack. In general, STEMIs are larger heart attacks than non-STEMIs, and the larger the size of the heart attack, the greater the chance of complications down the road such as heart failure.
Diagnosis
STEMI Protocol
A STEMI heart attack is diagnosed based on symptoms and the characteristic ECG pattern. The Heart Institute’s STEMI Regional Program has established a protocol to ensure that all STEMI patients in the region receive the best care as quickly as possible. If you call 911 with symptoms of a heart attack, trained paramedics will come and perform and interpret an ECG right away. If the diagnosis of STEMI is made, you will be transported directly to the Heart Institute or a designated centre for immediate treatment. If you arrive on your own to a local emergency department and the diagnosis of STEMI is made, you will be treated immediately according to protocols established by the Heart Institute.
Depending on your location, you will either be transported immediately to the Heart Institute or, if you are in more distant parts of the region, you will first be treated with medications that dissolve the clots (thrombolytics) and then transported to the Heart Institute.
The Heart Institute STEMI program has reduced STEMI deaths in the Ottawa region by 50%.
Non-STEMI
A non-STEMI heart attack does not present the same ECG pattern as a STEMI. This is because the artery is not completely blocked and the full thickness of the heart muscle is not being starved of oxygen-rich blood. In order to diagnose a non-STEMI, a chest X-ray, ECG, physical examination, special blood tests will be done. If heart cells have died, a protein (cardiac troponin) is released into the blood. Generally, it is a positive test for this protein that confirms the heart attack diagnosis.
Symptoms
A heart attack is just as likely to occur at rest as it is during exertion. Symptoms can include any of the following:
- Chest pain, often described as a tightness or heaviness
- Pain in the upper abdomen
- Pain in the back, neck, jaw, or arm
- Shortness of breath
- Sweating
- Nausea
- Loss of consciousness
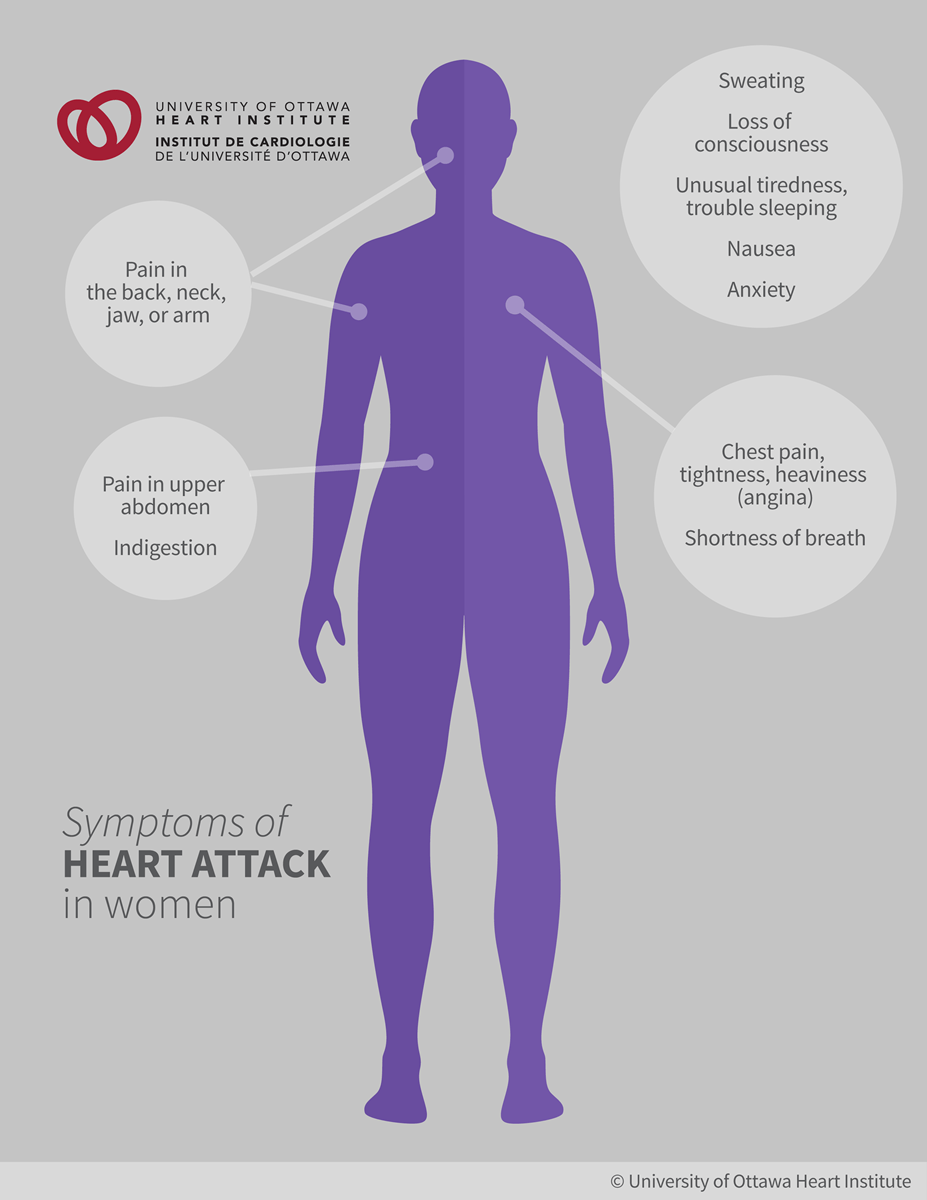
Women
Women can experience a heart attack differently than men. For some women, chest pain may not be the first sign of heart trouble. These women report less common symptoms, such as unusual tiredness, trouble sleeping, indigestion, and anxiety up to a month before the heart attack. Women with diabetes often have less common symptoms.
If you think you may be having a heart attack, call 911.
Treatments
Treatment: STEMI
The immediate treatment for a heart attack is to find the blocked artery and clear it as quickly as possible to restore normal blood flow.
There are two ways to do this. The first option is to perform an emergency angioplasty and stenting in which a small balloon and stent are inserted into the blocked artery. This is done via the wrist or the groin. The balloon is inflated at the blockage to open it mechanically, and the stent is left in place to hold the artery open. This treatment is successful in more than 90% of cases, but it can be performed only in specialized centres, such as the Heart Institute.
For people who live in the more distant parts of the Ottawa region, medication which dissolves clots is used. This medication can be administered in any emergency department. This is usually followed by immediate transport to the Heart Institute for specialized assessment and care.
In some cases, surgery called coronary artery bypass grafting (CABG) is required. This is a type of open heart surgery in which arteries from the chest or veins from the leg are used to bypass the narrowed portions of the heart arteries. This surgery is only performed in specialized centres, such as the Heart Institute.
Treatment: Non-STEMI
For non-STEMI heart attacks, initial treatment focuses on preventing the constricted artery from becoming completely blocked. Medications are given to keep the clot from growing and to allow it to dissolve on its own. This is followed by more testing to assess the risk of complications such as another heart attack.
An angiogram is usually the first test performed. This allows your doctor to directly view the arteries in your heart to see how much plaque has built up and where it is located. If large blockages are found, usually they will be treated by:
- Angioplasty and Stenting: A small balloon and stent is inserted via the wrist or the groin. The balloon is inflated in the blocked artery to open it mechanically. The stent is left in place to hold the artery open.
- Coronary Artery Bypass Grafting (CABG): Arteries from the chest, or veins from the leg, are used to bypass the narrowed portions of the heart arteries.
Non-invasive tests can include:
- Treadmill Testing: This test measures how well the heart functions when you are challenged to work harder than normal (for example, during exercise).
- Nuclear Perfusion Imaging: This imaging tool is used to identify areas of the heart that are receiving less blood than they should.
Lifestyle
Enrolment in a cardiac rehabilitation program is an ideal way to learn about changes that you can make to improve your quality of life and reduce your risk of suffering another heart attack. The aim is to encourage and support you while making change and to provide you with information about:
- Exercise
- Heart healthy diet
- Weight management
- Smoking cessation
- Stress management
Medications
Typically, five medications will be prescribed for you after your heart attack. You will probably be taking these medications for a long period of time. They include:
- ASA (Aspirin or other brands) to lower the risk of clots forming in your arteries
- Anti-platelet medications to lower the risk of another heart attack and to prevent clots from building up on stents
- Beta-blockers to reduce the workload of your heart and to improve heart function
- ACE inhibitors or angiotensin receptor blockers to lower the workload of your heart.
- Statins to lower cholesterol and the risk of another heart attack
These medications have been shown to lower the risk of another heart attack or of dying from a heart attack. Do not change or stop taking any of these medications without first discussing with your doctor.
Additional medications may be needed to control risk factors associated with heart disease, including high blood pressure and cholesterol, diabetes, and nicotine addiction. Nitroglycerine may also be prescribed at discharge in case a recurrence of chest pain occurs. Further medications may be required to treat some complications of heart attack, such as abnormal heart rhythms or heart failure.