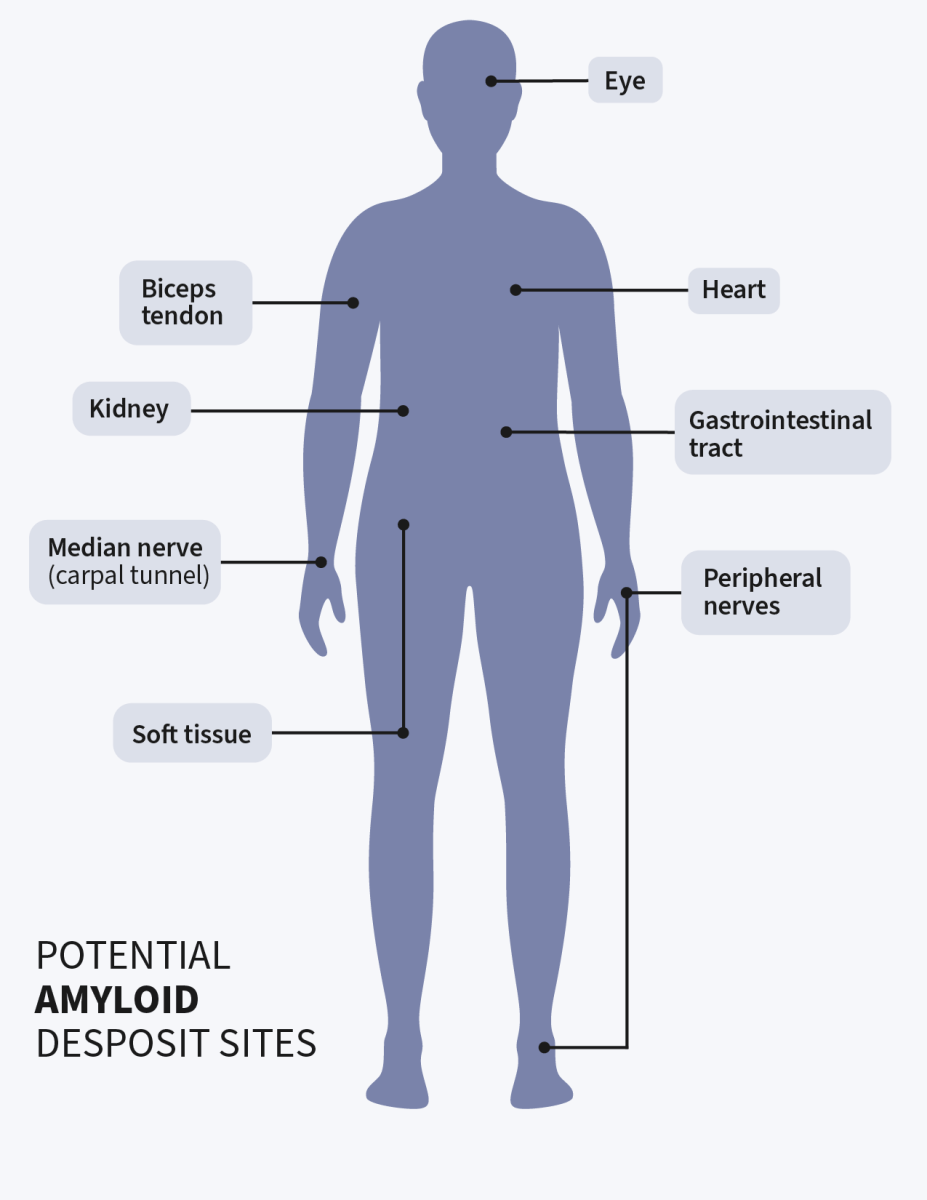
Amyloidosis is a rare, chronic condition in which abnormal proteins bunch together to form amyloid deposits. These deposits can build in certain body organs such as the heart, nerves, gastrointestinal tract, and kidneys, and may cause damage.
What is cardiac amyloidosis?
Cardiac amyloidosis is a rare condition caused by deposits of amyloid in the heart tissue. These deposits make it difficult for the heart to function properly, causing “stiff heart syndrome,” or restrictive cardiomyopathy. The walls of the lower heart chambers also become much thicker than usual. As a result, the heart does not fill properly and there is not enough blood to send throughout the body. This can result in congestive heart failure, which can occur when your heart is no longer strong enough to provide your body with all the blood and oxygen it needs. When this occurs, your heart works harder than usual and less efficiently.
Types of cardiac amyloidosis
There are two main types of amyloidosis that can affect your heart. It is important to identify the type as this will determine your treatment.
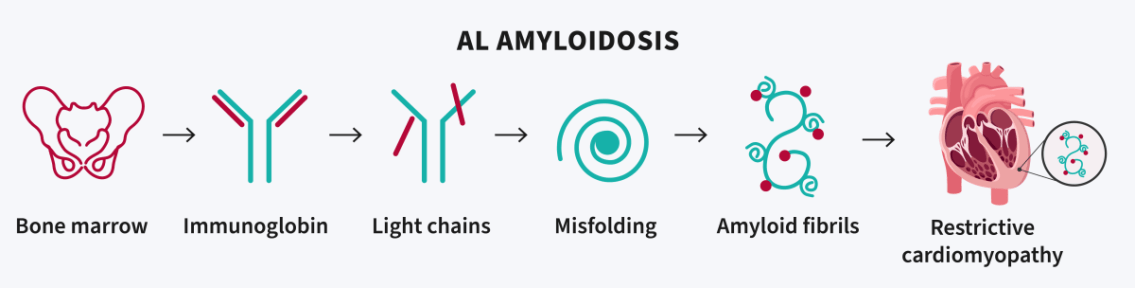
Amyloid light chain (AL)
This is a form of cancer, which starts in the bone marrow and mostly affects the heart and kidneys. The bone marrow makes too much of a light chain immunoglobin, which is then deposited in the body’s tissues. The light chain immunoglobin is normally used in fighting infections but, in this condition, the bone marrow makes too much. It is not known why the bone marrow makes too much AL. AL has an annual incidence of 10 in a million. It is generally a more rapidly progressing disease.
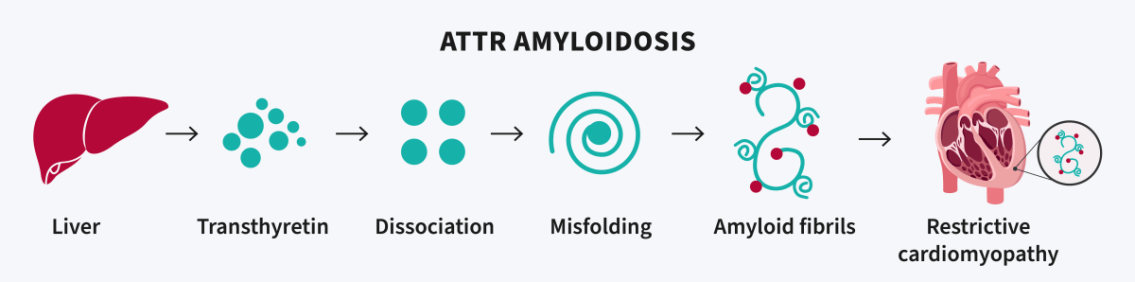
Transthyretin (TTR)
Caused by the liver, the TTR protein is typically involved with transporting thyroid hormone and retinol (vitamin A) in our bodies. Amyloidosis occurs when there is a misfolding of the TTR protein that then produces amyloid fibrils. There are two forms of TTR amyloidosis.
- Hereditary: This is caused by a change (known as a mutation) in a gene called TTR. This change can be passed down from parent to child and is diagnosed by genetic testing. It can affect family members in different ways. The two most common places for these deposits to build are in the heart and the nervous system. Deposits in the heart can lead to heart failure or abnormal heart rhythms. Deposits in the nervous system can lead to neurological symptoms, including numbness and tingling in the arms and legs.
- Wild type: This type develops for unknown reasons as people get older. It is more common than hereditary transthyretin amyloidosis (ATTR-CM). It most often develops in people over 65 years of age and is more common in men.
Both the hereditary and wild subtypes of transthyretin amyloidosis have an unknown prevalence and incidence and are a slowly progressing disorder.
On this page
Causes
Some people have hereditary transthyretin amyloidosis, which is caused by a change (known as a mutation) in a person’s genes. Otherwise, there is currently no known cause for why some people develop amyloidosis.
Diagnosis
Cardiac amyloidosis can be difficult to diagnose. The diagnosis may be suspected because of typical symptoms and the results of routine cardiac tests, such as:
- Blood work
- Electrocardiogram (ECG): A simple and painless test that measures and records the electrical activity of the heart.
- Echocardiogram (ECHO): An imaging technology that uses ultrasound to create images of your heart. It is a diagnostic test used to examine the heart and its blood supply, determine how large the heart is, how well it contracts, and how the valves function.
- Cardiac magnetic resonance imaging (MRI): A test performed to visualize the structure and function of the heart, valves and major arteries and veins.
Once suspected, other specialized tests are needed to confirm a diagnosis, including:
- Tissue biopsy: This test looks for the presence of amyloid protein. This is done by taking a small tissue sample.
- Pyrophosphate scan: A nuclear imaging technique used to determine whether a patient has AL or ATTR amyloidosis.
- Nuclear imaging: Positron emission tomography (PET) myocardial perfusion imaging (MPI) is an imaging process that shows how well blood flows to the muscle of the heart (myocardium).
- Genetic testing: Performed using a sample of blood a cardiologist has ordered. The blood sample is then examined by specialists. Only the TTR gene will be analyzed. None of the other 22,000 genes are analyzed.
Symptoms
Non-heart-related symptoms, such as carpel tunnel syndrome, joint, spine or nerve problems, can develop before heart problems in people with transthyretin amyloidosis cardiomyopathy.
Other symptoms can include problems with digestion, bowel or bladder function, vision, hearing and fatigue.
Treatments
Treatment for cardiac amyloidosis is based upon the specific type of condition present.
Symptoms
Symptoms are usually treated with medications that reduce swelling, support blood pressure, control heart rate and reduce stroke risk.
Light chain (AL)
Treatment includes chemotherapy and sometimes stem cell transplant. This is prescribed by a hematologist or an oncologist.
Transthyretin (ATTR)
Treatment includes medications that reduce amyloid protein build-up in the heart and/or nerves. The medication used depends on the type of ATTR (hereditary or wild type) and the symptoms a patient is experiencing.