Purpose
Patients who may need a transplant usually have one of two problems. One is irreversible damage to the heart because of coronary artery disease that has resulted in severe heart attacks or myocardial infarctions. The other problem is a heart muscle disease called cardiomyopathy, in which the heart is unable to contract normally because of damage to the muscle cells. Occasionally, other forms of heart disease require transplantation, such as congenital heart defects, which are structural problems present at birth.
Heart transplantation carries its own set of risks, including complications during or after the transplant, or death. A team of doctors and other health care professionals assesses all patients who are referred for transplant to determine who might benefit from the procedure. When a patient is accepted for a heart transplant, he or she is placed on a nationwide transplant waiting list. Patients are listed according to the severity of their medical condition, so sicker patients are generally given higher priority.
Description
- A wide range of tests are performed before the procedure.
- A nurse or doctor asks the patient to provide informed consent. This is required before the procedure is performed.
- The patient is placed under general anesthesia and remains unconscious for the entire operation.
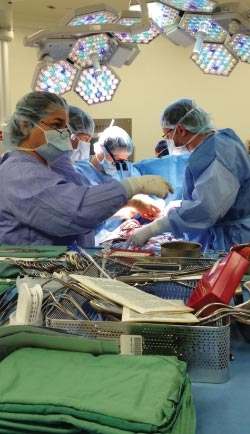
- The patient is taken by stretcher to the Cardiac Operating Room.
- Incisions (cuts) are made through the patient’s chest and breastbone to allow the surgeons access to the heart.
- The heart’s blood vessels are connected to a heart-lung machine (also called a heart-lung bypass machine), which pumps the patient’s blood through the body during the surgery.
- Once the heart-lung machine has taken over the patient’s circulation, the patient’s heart is removed from the chest.
- The surgeons sew the donor heart to the great vessels and remaining heart tissue of the patient.
- The new heart either starts beating automatically or is started with a small electrical shock. All incisions are then closed.
- The patient stays in the Cardiac Surgery Intensive Care Unit (CSICU) until well enough to be moved to a regular hospital bed. Anti-rejection medications are started after the surgery and must be continued for the rest of the patient’s life.
- The average hospital stay after a heart transplant is 14 days.
Patient instructions
While patients are waiting for a heart transplant, it is important that they are easily reachable by cell phone or pager at short notice. Patients living a long distance from the University of Ottawa Heart Institute may need to relocate to Ottawa as they wait for their transplants.
Additional info
Heart transplant recipients must take many different drugs, some for the rest of their lives. These drugs include:
- Immunosuppressants to shut down the body's natural immune responses that would damage the new heart
- Antibiotics, antivirals, and fungicides to fend off infection because the natural immune responses are disabled by the immunosuppressants
- Drugs to prevent coronary artery disease and regulate blood pressure
After a heart transplant, regular blood tests and tissue samples (biopsies) are taken from the heart to make sure the body is not rejecting the donor organ. Extra care should be taken to avoid exposure to germs that could cause illness because the immune system is not as strong as it was before the transplant.
For more information, see the Heart Transplant Patient Guide.

